Snoring Isn’t Just Annoying — It Could Be a Warning Sign of Sleep Apnea
Snoring Isn’t Just Annoying — It Could Be a Warning Sign of Sleep Apnea
Are You Ignoring the Signs?
Many people think snoring is harmless or simply an inconvenience for their bed partner. But loud, chronic snoring may actually be a warning sign of a serious sleep disorder called obstructive sleep apnea (OSA).
At Comprehensive Sleep Care Center, we help patients throughout Annapolis, Fairfax, Reston, Leesburg, Woodbridge, Alexandria, Frederick, Germantown, and surrounding communities identify and treat sleep apnea and other sleep disorders so they can sleep better and improve their overall health.
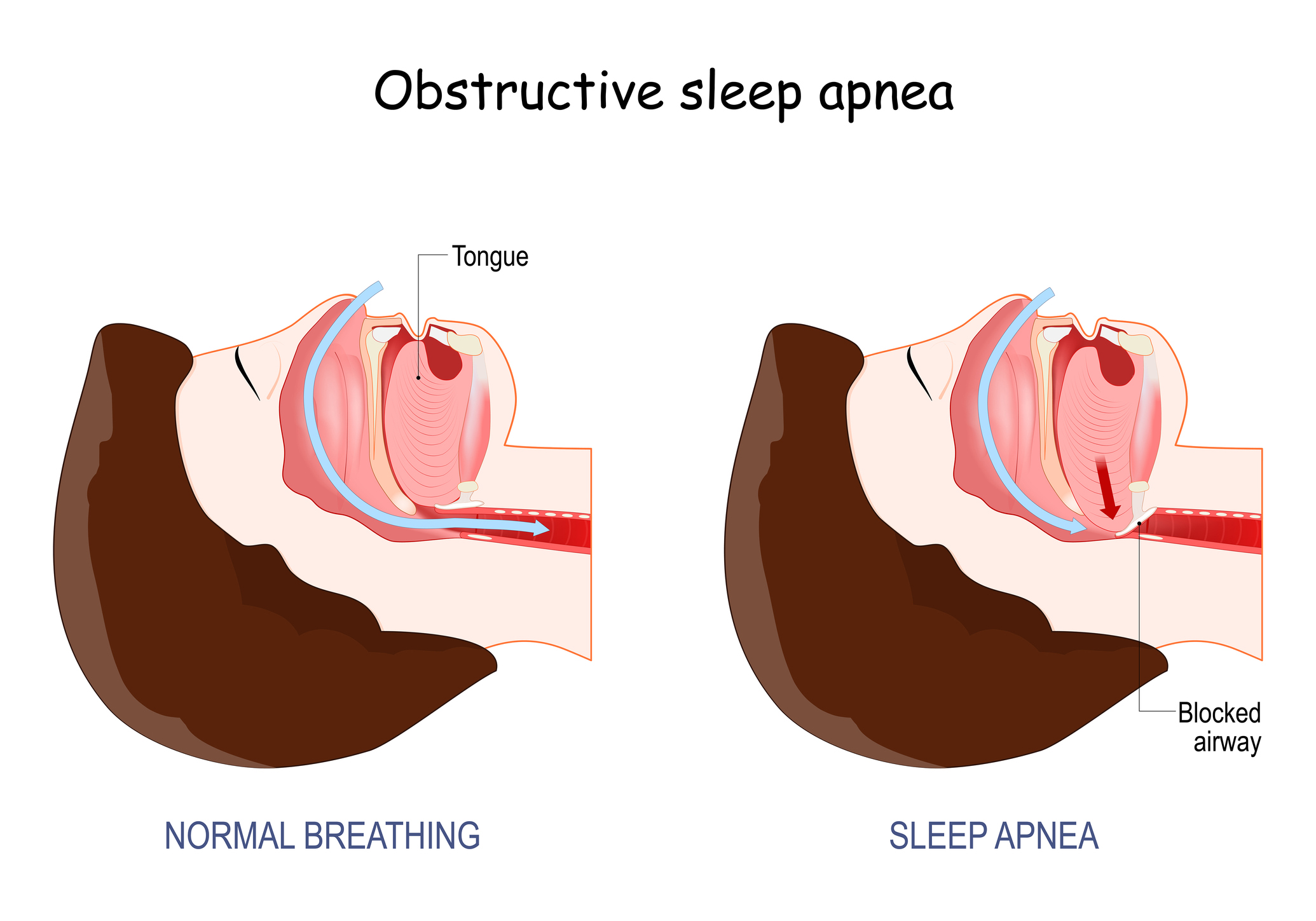
What Is Sleep Apnea?
Sleep apnea is a condition where breathing repeatedly stops and starts during sleep. The most common form, obstructive sleep apnea, occurs when the airway becomes blocked during sleep.
Many people with sleep apnea don’t even realize they have it.
Common Symptoms of Sleep Apnea:
- Loud snoring
- Gasping or choking during sleep
- Excessive daytime sleepiness
- Morning headaches
- Difficulty concentrating
- Irritability or mood changes
- Waking up feeling tired
- Dry mouth or sore throat in the morning
Why Snoring Shouldn’t Be Ignored
While not everyone who snores has sleep apnea, frequent loud snoring is one of the most common symptoms. Untreated sleep apnea can increase the risk of:
- High blood pressure
- Heart disease
- Stroke
- Diabetes
- Depression and anxiety
- Memory problems
- Fatigue-related accidents
Getting evaluated early can help prevent serious long-term health complications.
How Sleep Apnea Is Diagnosed
At Comprehensive Sleep Care Center, we offer convenient testing options including:
- Home Sleep Testing
- In-Lab Sleep Studies
- Comprehensive Sleep Evaluations
Our experienced sleep specialists work with patients to determine the best testing and treatment options based on their symptoms and health history.
Treatment Options for Sleep Apnea
There are several effective treatments available for sleep apnea, including:
- CPAP Therapy
- Oral Appliance Therapy
- Inspire Therapy referrals
- Lifestyle and sleep habit recommendations
- Personalized treatment plans
For patients who struggle with CPAP, Oral Appliance Therapy may provide a comfortable and effective alternative. And if seen by our in-house sleep medicine dentists it may be covered by your medical insurance (minus co-pay and deductible)
Sleep Better. Live Healthier.
Snoring may seem harmless, but it could be your body warning you about a more serious problem. If you or a loved one snores regularly, wakes up tired, or experiences daytime fatigue, it may be time for a sleep evaluation.
📞 Get evaluated today and take the first step toward better sleep and better health. Call or text “APT” to 703-729-3420.
Comprehensive Sleep Care Center proudly serves patients across Maryland, Virginia, West Virginia, and Washington, DC with 11 convenient locations including our new Annapolis office.