CPAP vs APAP
CPAP vs APAP
WHAT IS THE DIFFERENCE?
CPAP = CONTINUOUS POSITIVE AIRWAY PRESSURE
AUTOPAP, AUTOCPAP, OR APAP = AUTOMATIC POSITIVE AIRWAY PRESSURE
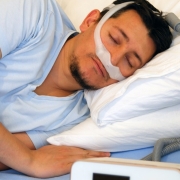
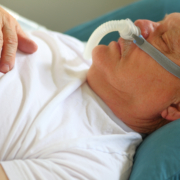
CPAPA vs APAP? We get a lot of questions on this and there is a lot of confusing information out there. When patients are diagnosed with Obstructive Sleep Apnea (OSA), the long-standing gold standard of treatment is Continuous Positive Airway Pressure (CPAP). For patients who cannot tolerate CPAP, the sleep medicine physician may try an Automatic Positive Airway Pressure or APAP.
The main difference between CPAP and APAP is how the air pressure is administered.
CPAP machines are set at a fixed pressure that is determined through an in-lab titration sleep study. The goal of an in-lab CPAP titration is to achieve a pressure setting where the patient demonstrates high-quality sleep, reduction in respiratory events by keeping the airway “propped” open while sleeping, and a consequent improvement in their circulating oxygen. An APAP, on the other hand, is given a range of pressures, rather than a single fixed pressure, and therefore has the ability to auto-adjust to the patient’s breathing. This option can be used when a patient’s recommended in-lab titration study is denied by the insurance carrier. Specifically, some CPAP machines available today include a new technology that allows the machine to change to a 30-day APAP mode. Once the 30 days are completed, the machine automatically selects a fixed pressure that is based upon the 90th percentile pressure administered to the patient through the machine during its APAP trial period. A dedicated APAP machine, however, may be more appropriate than a fixed CPAP for certain patients.
There is a lot of misleading information on the internet about CPAP vs APAP treatment.
It is important to note that much of the information is coming from the manufacturers of APAP machines and it may not be based on scientific research. Here at Comprehensive Sleep Care Center, we follow the guidelines of the American Academy of Sleep Medicine (AASM), not equipment manufacturers and distributors.
The below practice parameters are the most recent updates from the AASM regarding the use of auto-titrating positive airway pressure (APAP) devices for titrating pressures and treating adult patients with obstructive sleep apnea syndrome.
Continuous positive airway pressure (CPAP) at an effective setting verified by attended polysomnography {in-lab sleep study} is a standard treatment for obstructive sleep apnea (OSA). APAP devices change the treatment pressure based on feedback from various patient measures such as airflow, pressure fluctuations, or measures of airway resistance. These devices may aid in the pressure titration process, address possible changes in pressure requirements throughout a given night and from night to night, aid in treatment of OSA when attended CPAP titration {in-lab sleep study} has not or cannot be accomplished {insurance denial}, or to help improve patient comfort.
A task force of the Standards of Practice Committee of the American Academy of Sleep Medicine has reviewed the literature published since the 2002 practice parameter on the use of APAP.
CURRENT PAP RECOMMENDATIONS FOLLOW:
(1) APAP devices are not recommended to diagnose OSA
(2) patients with congestive heart failure, patients with significant lung disease such as chronic obstructive pulmonary disease; patients expected to have nocturnal arterial oxyhemoglobin desaturation due to conditions other than OSA (e.g., obesity hypoventilation syndrome); patients who do not snore (either naturally or as a result of palate surgery); and patients who have central sleep apnea syndromes are not currently candidates for APAP titration {sleep study}or treatment.
(3) APAP devices are not currently recommended for split-night titration {in-lab sleep study for OSA and if present the addition of PAP device to find appropriate settings}.
(4) certain APAP devices may be used during attended titration with polysomnography {in-lab sleep study} to identify a single pressure for use with standard CPAP for treatment of moderate to severe OSA.
(5) certain APAP devices may be initiated and used in the self-adjusting mode for unattended treatment of patients {at home use} with moderate to severe OSA without significant comorbidities {the simultaneous presence of two chronic diseases or conditions in a patient} (Congestive heart failure, COPD, central sleep apnea syndromes, or hypoventilation syndromes).
(6) certain APAP devices may be used in an unattended way to determine a fixed CPAP treatment pressure for patients with moderate to severe OSA without significant comorbidities (Congestive heart failure, COPD, central sleep apnea syndromes, or hypoventilation syndromes).
(7) patients being treated with fixed CPAP {set pressure} on the basis of APAP titration or being treated with APAP must have close clinical follow-up {follow up with sleep medicine office}to determine treatment effectiveness and safety.
(8) a re-evaluation and, if necessary, a standard attended CPAP titration study {in-lab sleep study} should be performed if symptoms do not resolve or the APAP treatment otherwise appears to lack efficacy.
https://aasm.org/resources/practiceparameters/pp_autotitrating.pdf