No Mask? No Problem. CPAP Alternatives for Sleep Apnea
No Mask? No Problem. CPAP Alternatives for Sleep Apnea
If you’ve been diagnosed with sleep apnea but struggle with wearing a CPAP mask, you’re not alone. Many patients find CPAP therapy uncomfortable, inconvenient, or difficult to maintain long-term. The good news? CPAP is not your only option.
At Comprehensive Sleep Care Center (CSCC), we offer effective CPAP alternatives designed to help you sleep better—without the mask.
Why CPAP Isn’t for Everyone
CPAP therapy is highly effective, but some patients experience challenges such as:
-
Mask discomfort or claustrophobia
-
Dry mouth or nasal irritation
-
Difficulty sleeping on your side
-
Trouble traveling with equipment
-
Poor long-term compliance
If CPAP hasn’t worked for you, that doesn’t mean your sleep apnea can’t be treated.
CPAP Alternatives Available at CSCC
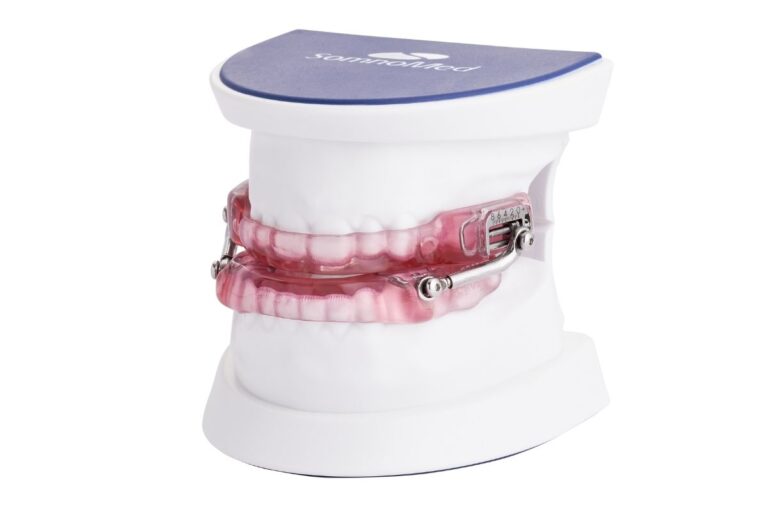
Oral Appliance Therapy (OAT)
Oral Appliance Therapy is a comfortable, custom-made dental device worn while you sleep. It gently repositions the jaw to keep your airway open and reduce apneas.
Benefits of Oral Appliance Therapy:
-
Small, quiet, and portable
-
No mask or tubing
-
Ideal for mild to moderate obstructive sleep apnea
-
Great option for frequent travelers
-
Custom-fitted
- Covered by most insurances when seen by our in-house sleep medicine dentists
Many patients find oral appliances easier to use and more comfortable than CPAP—leading to better consistency and improved sleep.
Inspire® Therapy
Inspire® is an FDA-approved implantable treatment for moderate to severe obstructive sleep apnea in patients who cannot tolerate CPAP.
How Inspire Works:
-
A small device is implanted during an outpatient procedure
-
It stimulates airway muscles to keep the airway open during sleep
-
Controlled with a handheld remote
-
No mask, no hose, no noise
Inspire therapy works with your body’s natural breathing patterns and has helped thousands of patients regain restful sleep.
How CSCC Helps You Find the Right Solution
At Comprehensive Sleep Care Center, we take a personalized approach to sleep apnea treatment. Our board-certified sleep specialists will:
-
Review your sleep study results
-
Discuss your CPAP experience and concerns
-
Evaluate your eligibility for CPAP alternatives
-
Create a treatment plan tailored to your lifestyle and medical needs
Whether you’re newly diagnosed or looking for a better solution, we’re here to help.
Sleep Better—Your Way
Sleep apnea is a serious condition, but treatment doesn’t have to feel impossible. If CPAP isn’t working for you, there are proven alternatives that may fit your life better.
No mask? No problem. Let CSCC help you find the right path to better sleep and better health.
👉 Schedule a consultation today at www.comprehensivesleepcare.com
Comprehensive Sleep Care Center is proud to serve patients at the following locations: